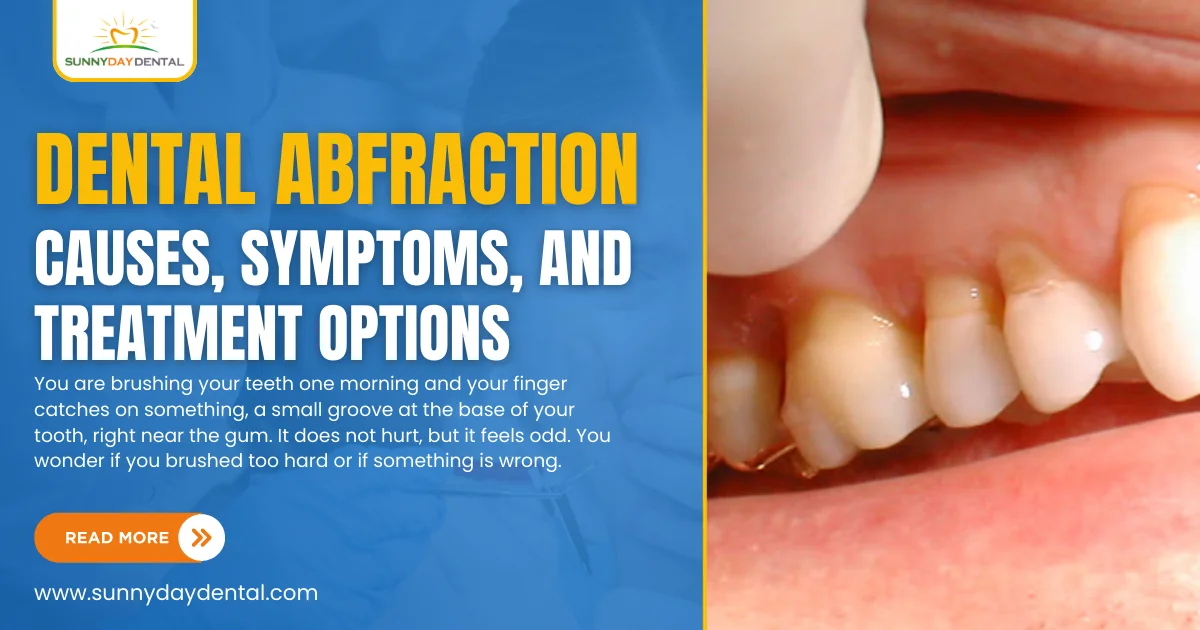
You are brushing your teeth one morning and your finger catches on something, a small groove at the base of your tooth, right near the gum. It does not hurt, but it feels odd. You wonder if you brushed too hard or if something is wrong. Those little notches near the gumline could be a sign of dental abfraction, and it deserves your attention.
Table of Contents
ToggleDental abfraction is more common than most people realize, and yet it is one of the most misunderstood dental conditions out there. Many patients confuse it with cavities or gum disease. The truth is, it is its own condition with its own causes, and thankfully, its own solutions. Let’s break it all down for you in plain, simple language.
What is Dental Abfraction?
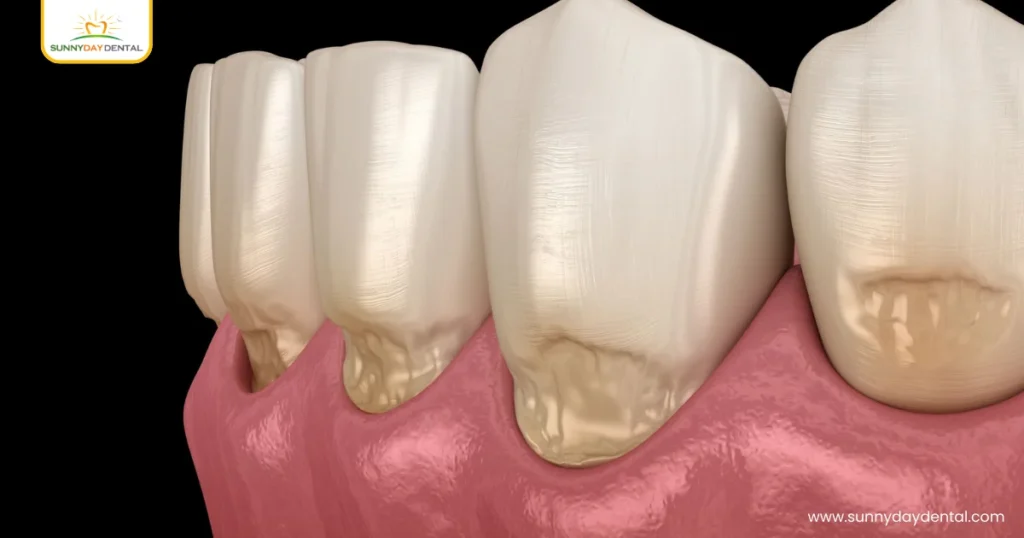
It refers to the wearing away of tooth structure at the point where the tooth and gum meet. Think of your tooth like a tree. If the trunk is under constant stress from strong winds, it eventually begins to weaken and crack at the base. The same thing happens to your teeth when they experience repeated pressure from biting, chewing, or grinding.
Unlike a cavity, It is not caused by bacteria or sugar. It is a mechanical problem, meaning it comes from the physical forces your teeth deal with every single day. The result is a small, wedge-shaped notch near the gumline that can grow deeper over time if nothing is done about it.
Dental Abfraction Definition (Quick Overview)
Dental abfraction is the loss of tooth structure at the gumline, caused by excessive biting forces that stress the tooth. This leads to small notches or grooves forming where the tooth meets the gum. They develop slowly over time and can cause sensitivity, discomfort, and long-term damage if left untreated.
What Causes Dental Abfraction?
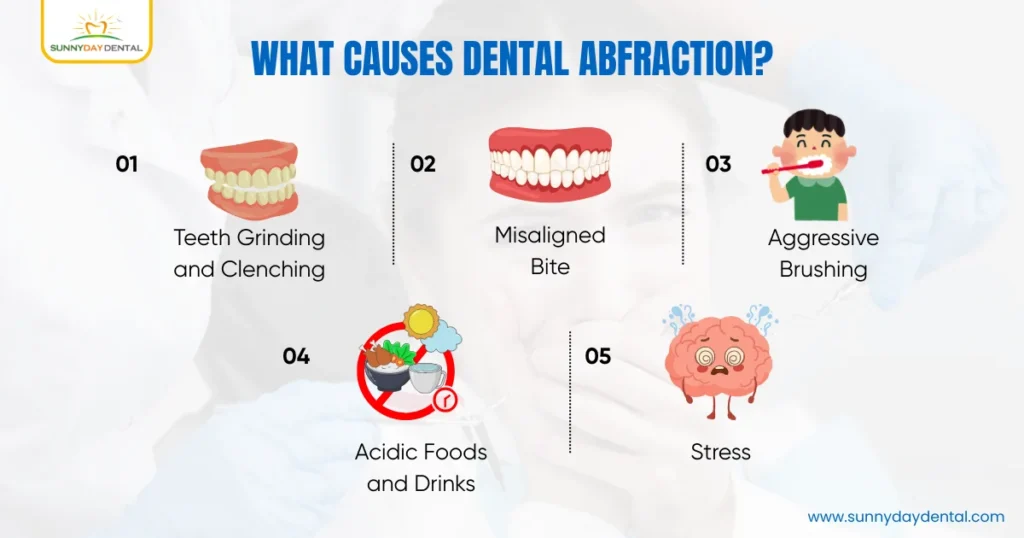
It begins with stress concentration at the base of the tooth. When you bite down unevenly or grind your teeth, the pressure does not distribute evenly. Instead, it builds up at the neck of the tooth, which is the most vulnerable part, leading to gradual structural breakdown.
1. Teeth Grinding and Clenching: Constant grinding is one of the leading causes of abfraction teeth. Over months and years, the enamel at the base simply wears away.
2. Misaligned Bite: When your upper and lower teeth do not line up correctly, some teeth take on more force than they should. This uneven load puts specific teeth at much higher risk.
3. Aggressive Brushing: Brushing too hard or using a hard-bristled toothbrush can worsen existing notches near the gumline and accelerate the loss of tooth structure.
4. Acidic Foods and Drinks: While acid does not cause abfraction directly, it softens enamel, making it far more vulnerable to mechanical wear.
5. Stress: Higher stress levels often translate to more grinding and clenching, which in turn speeds up abfraction teeth.
The important takeaway here is that dental abfraction is rarely caused by just one thing. It is usually a combination of habits and bite-related issues working together. Knowing your personal risk factors helps your dentist create a treatment plan that actually works for you.
4 Signs and Symptoms You Should Not Ignore

Dental abfraction does not always announce itself with pain. In fact, many people have it for years before noticing. Your mouth is always giving you signals. The challenge is learning to read them.
1. Notches near gumline: Small, wedge-shaped grooves at the base of one or more teeth are the most recognizable sign of abfraction teeth.
2. Tooth Sensitivity: A sharp reaction to hot, cold, sweet, or even air can indicate that the protective enamel has worn away at the base.
3. Visible Indentations: You may be able to see or feel a dip or groove at the point where your tooth meets your gum.
4. Gum Recession: As the notch deepens, the surrounding gum may begin to pull back, exposing more of the tooth root.
Ignoring these symptoms allows dental abfraction to progress to the point where the tooth becomes structurally weak or even at risk of fracturing. Early action is always the smarter move.
How is Dental Abfraction Diagnosed?
A dentist can identify dental abfraction during a routine checkup. They will look at the shape and location of the notch, assess your bite, and ask about habits like grinding or clenching. X-rays help to see how much of the tooth structure has been affected beneath the surface.
Difference Between Abfraction and Abrasion
Although abfraction and abrasion both cause damage near the gumline, they have different causes and require different treatment approaches.
Dental abfraction is caused by excessive biting forces and tooth stress. These forces cause the tooth structure to weaken and form wedge-shaped notches at the gumline. Grinding, clenching, and bite misalignment are the most common causes.
Dental abrasion, on the other hand, is caused by external mechanical wear. This typically happens due to aggressive tooth brushing, using a hard-bristled toothbrush, or improper brushing technique. Abrasion usually results in smoother, more rounded wear areas rather than sharp notches.
Here is a simple comparison:
- Cause:
Abfraction: Bite pressure and tooth stress
Abrasion: Aggressive brushing or external friction - Shape of damage:
Abfraction: Sharp, wedge-shaped notch
Abrasion: Smooth, rounded wear - Location:
Both occur near the gumline - Treatment:
Abfraction: Bite correction, night guards, bonding
Abrasion: Brushing correction, soft toothbrush, bonding if severe
A dentist in Woodbridge can properly diagnose the cause and recommend the most effective treatment to protect your teeth.
5 Abfraction Treatment Options: What Works Best?
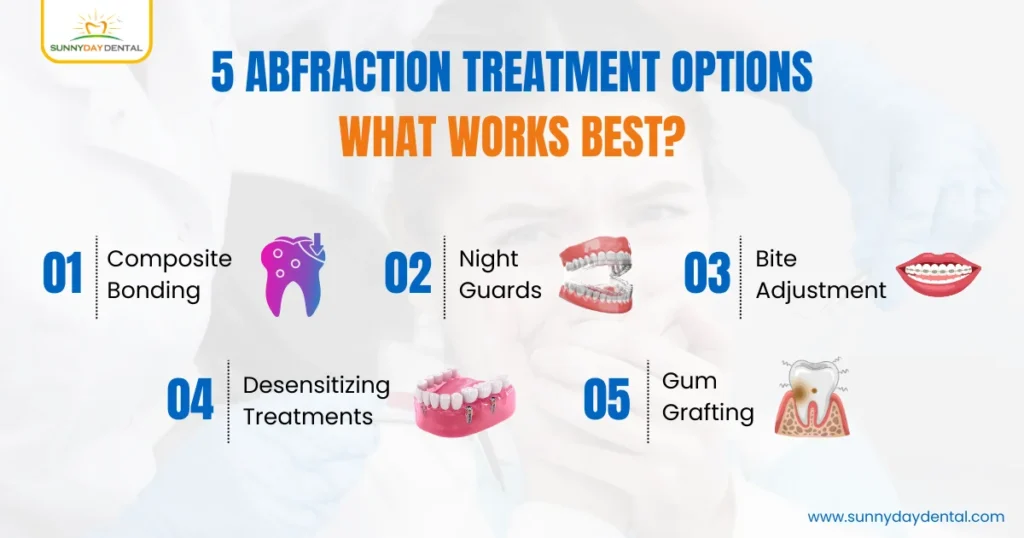
The good news is that dental abfraction is very treatable, especially when caught early. Your dentist in Woodbridge will recommend a treatment plan based on how severe the notch is and what is causing it. Abfraction treatment is not a one-size-fits-all solution. Here is what modern dentistry offers:
1. Composite Bonding: For mild to moderate notches, your dentist can fill the groove with tooth-colored composite resin. This restores the shape of the tooth and protects the exposed area from further wear.
2. Night Guards: If grinding or clenching is the culprit, a custom-made night guard worn while sleeping absorbs the pressure before it can damage your teeth further.
3. Bite Adjustment: In cases where a misaligned bite is the underlying issue, your dentist may reshape certain teeth slightly or recommend orthodontic treatment to redistribute the forces more evenly.
4. Desensitizing Treatments: For patients experiencing significant sensitivity, fluoride varnishes or desensitizing agents can provide relief while protecting the exposed tooth surface.
5. Gum Grafting: In advanced cases where gum recession has occurred alongside abfraction, a gum graft may be necessary to restore coverage and protect the root.
The most effective treatment addresses both the symptom and the cause – meaning the grinding, bite issue, or brushing habit. Treating one without the other often leads to the problem resurfacing.
How to Prevent Dental Abfraction
Prevention is always better than treatment. Use a soft-bristled toothbrush and gentle circular motions when brushing. Get your bite evaluated if you suspect misalignment. Wear a night guard if you grind your teeth. Cut down on acidic foods and drinks. And never skip your dental checkups, because a dentist can catch the early signs of dental abfraction before they become a bigger problem.
Treat Your Dental Abfraction Today With Sunny Day Dental

If any of what you just read sounds familiar, do not wait. Notches near gumline are not just a cosmetic concern. They are a signal that your teeth need attention. Sunny Day Dental, your trusted dentist in Woodbridge, is here to help you take action and protect your smile for the long term.
- Book a Dental Abfraction Assessment: Schedule a dedicated appointment to evaluate the condition of your teeth, bite alignment, and gum health so we can catch any issues early.
- Ask About Custom Night Guards: If grinding is contributing to your abfraction teeth, our team will fit you with a comfortable, custom night guard designed specifically for your bite.
- Explore Tooth-Colored Bonding: Find out if composite bonding is right for your notches and how quickly we can restore the look and function of your affected teeth.
- Get a Bite Analysis: Our dentist in Woodbridge will assess whether your bite pattern is putting excessive stress on specific teeth and recommend the best corrective approach.
At Sunny Day Dental, we believe that every patient deserves clear answers and comfortable care. Whether you are experiencing sensitivity, noticing changes near your gumline, or simply want to be proactive about your dental health, we are ready to support you every step of the way.
FAQs About Dental Abfraction
1. Can dental abfraction heal on its own without treatment?
No, dental abfraction does not heal on its own. The loss of tooth structure from abfraction is permanent. That is why getting a proper evaluation and treatment from a dentist is so important.
2. Is dental abfraction the same as a cavity?
A cavity is caused by bacteria producing acid that dissolves tooth structure, typically on the biting surface or between teeth. Dental abfraction, on the other hand, is caused by stress at the base of the tooth.
3. Can children get dental abfraction?
It is possible in children, particularly those who grind their teeth heavily. However, because children’s teeth are still developing and they eventually lose their baby teeth, the long-term impact is less concerning.
4. How long does abfraction treatment take to complete?
This depends entirely on the condition and the treatment chosen. A simple composite bonding procedure can be completed in a single appointment. More complex cases involving bite correction may take over weeks or months.
5. Will my dental insurance cover my treatment?
Coverage varies widely depending on your insurance plan and the type of treatment required. Some plans cover composite bonding as a restorative procedure, while others may classify it as cosmetic and not cover it.